Interventional Treatment of Spine, Ligament, and Joint Injuries Using PRP
In the world of regenerative medicine, Platelet-Rich Plasma (PRP) therapy has emerged as a game-changer for treating injuries to the spine, ligaments, and joints. This minimally invasive approach harnesses the body's own healing powers to accelerate recovery, reduce pain, and potentially avoid more aggressive interventions like surgery.
Whether you're dealing with chronic back pain, a torn ligament from sports, or joint degeneration due to arthritis, PRP injections offer a promising option. In this blog post, we'll dive into what PRP is, how it's used in interventional treatments, its applications for specific injuries, benefits, risks, and what to expect. Remember, this is general information—consult a specialist for advice tailored to your situation.
## What is PRP and How Does It Work?
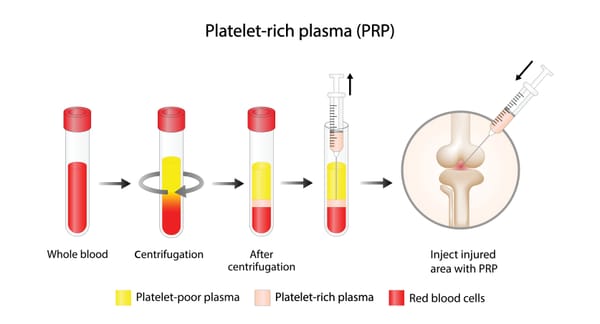
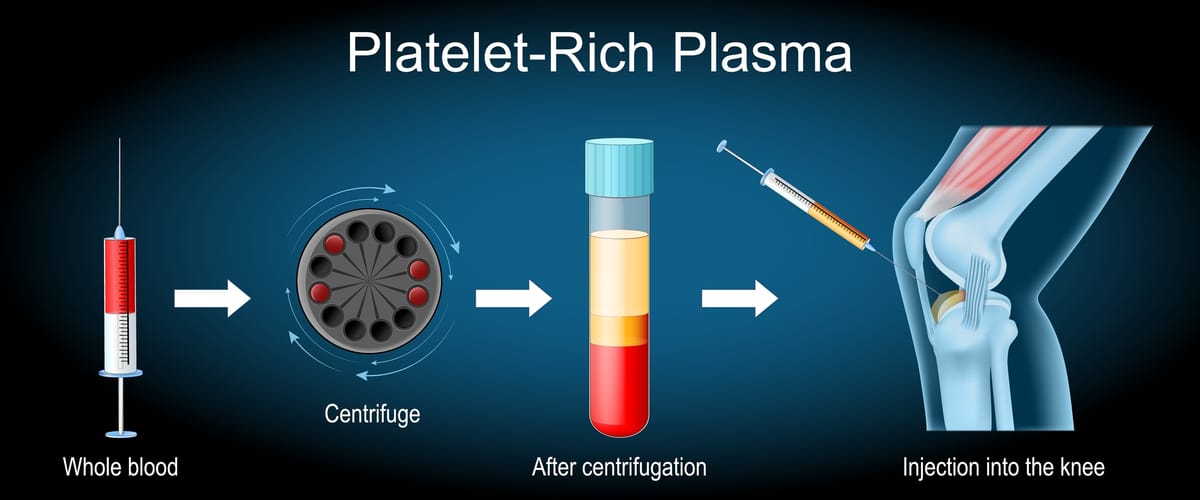
Platelet-Rich Plasma is derived from your own blood. The process starts with a simple blood draw, similar to a routine lab test. The blood is then spun in a centrifuge to separate the components, concentrating the platelets—which are packed with growth factors, proteins, and cytokines that promote tissue repair and reduce inflammation. These growth factors stimulate cell regeneration, enhance blood flow, and support the healing of damaged tissues like tendons, ligaments, cartilage, and even spinal discs.
In interventional treatments, PRP is injected directly into the injured area under imaging guidance, such as ultrasound or fluoroscopy, to ensure precision. This targeted delivery maximizes effectiveness while minimizing risks. Unlike traditional pain management with steroids, PRP focuses on regeneration rather than just symptom relief, making it a popular choice in orthopedics and pain medicine.
## PRP for Spine Injuries
Spinal injuries, including disc herniations, degenerative disc disease, and facet joint arthritis, can cause debilitating pain and mobility issues. PRP therapy is increasingly used here as an interventional option to promote healing and alleviate symptoms.
For example, in cases of spinal arthritis or disc-related pain, PRP injections can be administered into the affected discs or facet joints to reduce inflammation and encourage tissue repair. Recent advances show PRP's regenerative capabilities in repairing spinal tissues, potentially improving outcomes for conditions like discitis or chronic back pain. Neck and back pain from degenerative changes also respond well, with PRP helping to stabilize the spine by supporting ligament and muscle recovery.
The procedure is typically outpatient, with patients experiencing gradual improvement over weeks as the growth factors kick in.
## PRP for Ligament Injuries
Ligaments are the tough bands connecting bones, and injuries like tears or sprains—common in knees (ACL, MCL), ankles, or shoulders—can sideline athletes and active individuals. PRP accelerates ligament healing by concentrating platelets at the injury site, promoting collagen production and tissue strength.
Studies highlight PRP's benefits in augmenting tendon and ligament repair, with positive effects at molecular and cellular levels. For torn ligaments, PRP reduces inflammation, alleviates pain, and enhances vascularization, potentially improving stability post-reconstruction. It's particularly effective for partial tears or chronic instabilities, often injected under ultrasound guidance to target the exact ligament.
Compared to rest or physical therapy alone, PRP can speed up return to activity, making it a go-to for sports medicine.
## PRP for Joint Injuries
Joint injuries, from osteoarthritis to acute trauma, affect millions, leading to pain, swelling, and reduced function. PRP injections revolutionize joint treatment by tackling inflammation, restoring tissue health, and promoting regeneration.
In knees, shoulders, hips, or elbows, PRP is injected into the joint space to support cartilage repair and lubricate the area, especially useful for mild to moderate arthritis or post-injury recovery. It stabilizes joints by strengthening surrounding ligaments and tendons, helping heal faster and reducing the need for invasive procedures. For conditions like plantar fasciitis or mild sprains involving joints, PRP concentrates repair efforts for quicker recovery.
Results are often noticeable after several weeks, with sustained benefits for months.
## Benefits and Risks of PRP Therapy
The appeal of PRP lies in its natural approach—using your own blood minimizes allergic reactions and is generally safe. Benefits include faster healing, pain reduction, improved function, and potentially delaying surgery. It's versatile for spine, ligaments, and joints, with minimal downtime—most return to light activities quickly.
However, risks exist: temporary soreness at the injection site, infection (rare), or variable results since not all injuries respond equally. Evidence is promising but mixed; while many studies show benefits, more research is needed for long-term efficacy. Insurance coverage varies, as PRP is sometimes considered experimental.
## What to Expect from PRP Treatment
A typical session involves blood draw, processing (about 30 minutes), and injection under guidance. Multiple sessions may be needed, spaced weeks apart. Post-treatment, rest the area initially, then incorporate physical therapy for optimal results.
If you're considering PRP for spine, ligament, or joint issues, discuss with an interventional pain specialist or orthopedist. They can assess if it's right for you based on imaging and history.
## Final Thoughts
PRP therapy represents a shift toward regenerative, patient-centered care for spine, ligament, and joint injuries. By leveraging your body's healing potential, it offers hope for faster, more natural recovery. While not a cure-all, its growing use in interventional medicine underscores its value.