Understanding Joint Pain: Causes, Generators, and Interventional Treatment Options
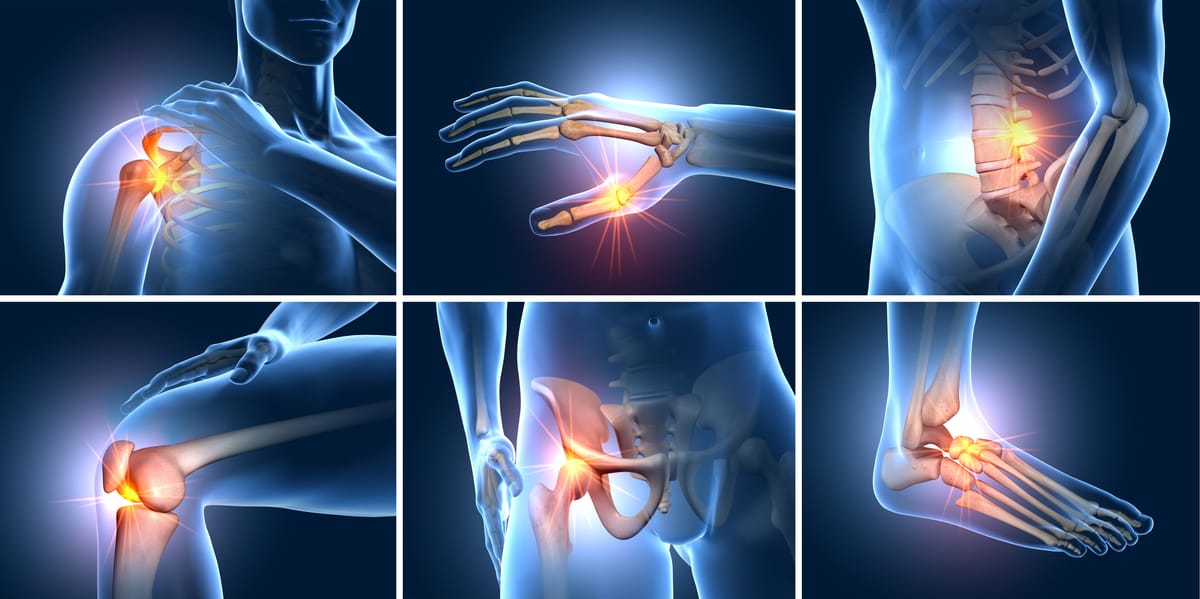
Joint pain is a common complaint that affects millions of people worldwide, limiting mobility and impacting quality of life. Whether it's a nagging ache in your shoulder after a workout or sharp discomfort in your knee while climbing stairs, understanding the underlying causes—known as pain generators—and available treatments can empower you to seek relief. In this post, we'll explore pain in major joints like the shoulder, knee, hip, and elbow, dive into potential pain generators, and discuss interventional approaches that go beyond basic pain meds or rest. Remember, this isn't medical advice—always consult a healthcare professional for personalized guidance.
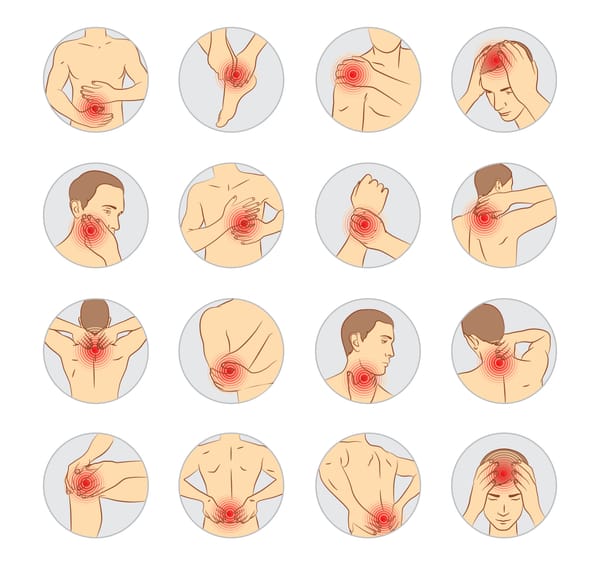
What Are Pain Generators in Joints?
Pain generators refer to the specific structures or conditions within or around a joint that trigger discomfort. Joints are complex systems involving bones, cartilage, ligaments, tendons, muscles, and fluid-filled sacs called bursae. When any of these components become inflamed, damaged, or irritated, pain ensues.Common pain generators include:
- Arthritis: Osteoarthritis (wear-and-tear) is the most frequent culprit, causing cartilage breakdown and bone-on-bone friction. Rheumatoid arthritis, an autoimmune condition, leads to joint inflammation and swelling.
- Bursitis: Inflammation of the bursae, often from overuse, commonly affects the shoulder, elbow, hip, and knee. This can cause swelling, stiffness, and pain that worsens with movement.
- Tendinitis: Overuse or injury inflames tendons, leading to pain in areas like the rotator cuff (shoulder) or Achilles tendon (near the ankle, but relevant for knee/hip mechanics).
- Injuries: Sprains, strains, fractures, or tears (e.g., meniscus in the knee or labrum in the hip) from trauma or repetitive stress.
- Other Factors: Infections, gout (crystal buildup in joints), or referred pain from nearby structures like the spine. Synovitis (inflammation of the joint lining) is another key generator in conditions like osteoarthritis.
These generators often overlap; for instance, arthritis might lead to secondary bursitis. Pain can also stem from muscle imbalances, poor posture, or even metabolic issues.
Joint-Specific Pain: Generators and Examples
Let's break it down by joint, focusing on the most common ones.
Shoulder Pain
The shoulder is a ball-and-socket joint with a wide range of motion, making it prone to issues. Common generators:
- Rotator cuff tendinitis or tears from overhead activities.
- Frozen shoulder (adhesive capsulitis), causing stiffness and pain.
- Bursitis or impingement syndrome, where tendons rub against bone.
Symptoms often include pain when lifting arms or sleeping on the affected side.
Knee Pain
As a weight-bearing hinge joint, the knee absorbs significant stress. Key generators:
- Osteoarthritis, especially in older adults, leading to cartilage loss.
- Meniscus tears or ligament injuries (e.g., ACL) from sports or twists.
- Patellofemoral pain syndrome (runner's knee) from misalignment or overuse.
- Bursitis or tendinitis around the kneecap.
Pain might worsen with squatting, stairs, or prolonged sitting.Hip PainThe hip, another ball-and-socket joint, supports body weight and enables walking. Generators include:
- Osteoarthritis or avascular necrosis (bone death from poor blood supply).
- Trochanteric bursitis on the outer hip.
- Labral tears or hip impingement, common in athletes.
Discomfort often radiates to the groin, thigh, or buttocks.
Elbow Pain
The elbow acts as a hinge for arm movement. Common issues:
- Tennis elbow (lateral epicondylitis) or golfer's elbow (medial epicondylitis) from repetitive gripping.
- Bursitis at the tip of the elbow.
- Arthritis or nerve entrapment, like cubital tunnel syndrome.
Pain typically flares with bending, lifting, or twisting motions.
Interventional Treatment Approaches
When conservative treatments like rest, ice, physical therapy, or over-the-counter anti-inflammatories fall short, interventional procedures offer targeted relief. These are minimally invasive techniques performed by interventional pain specialists, under imaging guidance for precision.
Corticosteroid Injections
- How it works: A steroid mixed with a local anesthetic is injected into the joint, bursa, or tendon sheath to reduce inflammation.
- Best for: Bursitis, tendinitis, or arthritis flares in shoulders, knees, hips, or elbows.
- Pros/Cons: Quick relief (lasting weeks to months), but repeated use can weaken tissues. Not ideal for long-term management.
Hyaluronic Acid Injections (Viscosupplementation)
- How it works: Synthetic joint fluid is injected to lubricate and cushion, mimicking natural synovial fluid.
- Best for: Knee or hip osteoarthritis where cartilage is thinning.
- Pros/Cons: Can improve mobility for 6-12 months; side effects are rare but include temporary swelling.
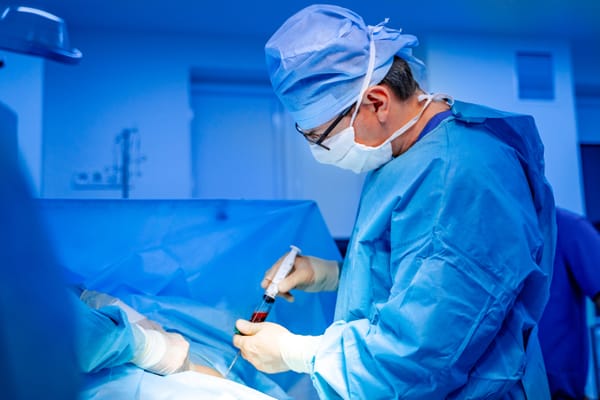
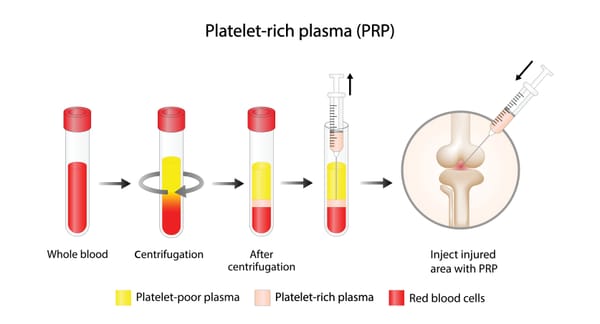
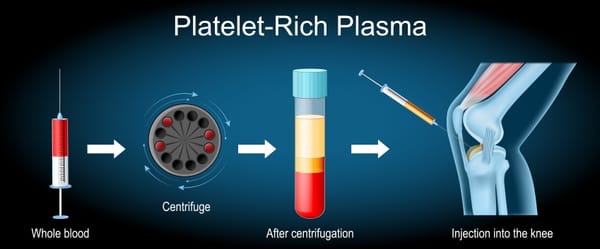
Platelet-Rich Plasma (PRP) Therapy
- How it works: Blood is drawn, spun to concentrate platelets (growth factors), and injected into the damaged area to promote healing.
- Best for: Tendinitis, partial tears, or mild arthritis in shoulders, knees, or elbows.
- Pros/Cons: Uses your body's own cells for regeneration; evidence is promising but variable. Multiple sessions may be needed.
Radiofrequency Ablation (RFA)
- How it works: Heat from radio waves disrupts pain-transmitting nerves around the joint.
- Best for: Chronic arthritis pain in knees, hips, or shoulders when other injections fail.
- Pros/Cons: Relief can last 6-18 months; minimally invasive, but nerves may regenerate over time.
Arthrocentesis (Joint Aspiration)
- How it works: Fluid is drained from swollen joints to relieve pressure, often combined with injections.
- Best for: Gout, infections, or effusions in knees or shoulders.
- Pros/Cons: Immediate relief; risks include infection if not sterile.
Advanced Options: Stem Cell Therapy or Prolotherapy
- Stem Cells: Harvested from bone marrow or fat, injected to potentially regenerate tissue. Emerging for osteoarthritis but still investigational.
- Prolotherapy: Irritant solutions injected to stimulate ligament/tendon repair. Useful for instability-related pain.
Before any procedure, imaging like X-rays, MRI, or ultrasound helps identify the exact pain generator. Success rates vary by condition and individual factors like age or activity level.
Final Thoughts
Joint pain doesn't have to sideline you forever. By pinpointing pain generators and exploring interventional treatments, many find significant improvement. Lifestyle tweaks—weight management, exercise, and ergonomics—complement these approaches. If pain persists, see a specialist to tailor a plan.