Understanding Spine Biopsy Under Imaging Guidance: Disc and Bone Procedures
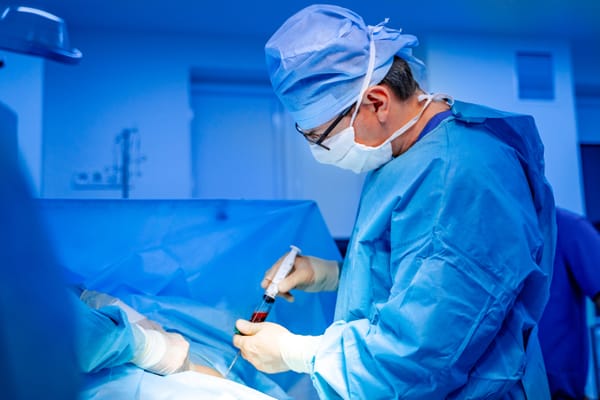
Spine biopsies are essential diagnostic tools in modern medicine, allowing doctors to sample tissue from the spinal discs or bones to identify infections, tumors, or other abnormalities. Performed under imaging guidance like CT, fluoroscopy, or ultrasound, these minimally invasive procedures offer precision while minimizing risks compared to open surgery.
Whether it's investigating unexplained back pain, confirming cancer metastasis, or diagnosing discitis (inflammation of the intervertebral disc), a spine biopsy can provide crucial insights. In this post, we'll explore what these procedures entail, why they're done, how they're performed, potential risks, benefits, and recovery. As always, this is for informational purposes—consult a healthcare professional for personalized advice.
What is a Spine Biopsy?
A spine biopsy involves removing a small sample of tissue from the spinal column for laboratory analysis. There are two main types:
- **Bone Biopsy**: Targets the vertebral bones to evaluate abnormalities like fractures, tumors (benign or malignant), infections (osteomyelitis), or inflammatory conditions. It's often used when imaging shows suspicious lesions.
- **Disc Biopsy**: Focuses on the intervertebral discs, commonly for suspected infectious discitis, where bacteria or fungi cause inflammation and pain. This helps identify the causative organism for targeted treatment.
These procedures are typically percutaneous (through the skin) and guided by real-time imaging to ensure accurate needle placement, avoiding vital structures like nerves or blood vessels.
## Why is a Spine Biopsy Performed?
Doctors recommend a spine biopsy when other tests, like blood work or imaging (MRI, CT, or bone scans), suggest an issue but can't confirm it. Common indications include:
- Investigating bone pain, tenderness, or unexplained fractures.
- Differentiating between benign and malignant tumors, or checking for metastasis in cancer patients.
- Diagnosing infections like discitis, osteomyelitis, or tuberculosis, especially if blood cultures are negative.
- Evaluating for recurrence of tumors or non-specific lesions on imaging.
- Ruling out malignancy in vertebral compression fractures.
For infectious discitis, biopsies are key to identifying pathogens like bacteria or mycobacterium tuberculosis, guiding antibiotic therapy.
## Preparation for the Procedure
Proper preparation ensures safety and effectiveness. Here's what to expect:
- **Medical Review**: Your doctor will take a full history, perform a physical exam, and order blood tests to check clotting and infection risks. Inform them of allergies, medications (especially blood thinners like aspirin or warfarin, which may need to be paused), and any pregnancy concerns, as radiation from imaging could affect the fetus.
- **Fasting**: Avoid eating for 6-8 hours beforehand; clear fluids may be allowed up to 2 hours prior.
- **Logistics**: Arrange transportation home, as sedation might be used. Wear comfortable clothing and remove jewelry.
If you're an outpatient, you'll be admitted briefly for monitoring.
## The Procedure: Step-by-Step
Spine biopsies are usually outpatient, lasting 30-60 minutes, and performed by a radiologist or interventional specialist. Imaging guidance—primarily CT for its precision, but also fluoroscopy or ultrasound—allows real-time visualization.
1. **Positioning and Setup**: You'll lie prone (face down) for most thoracic/lumbar procedures or supine/lateral for cervical ones. Vital signs are monitored, and an IV may deliver sedation or fluids.
2. **Anesthesia**: The skin is cleaned and numbed with local anesthetic (which may sting briefly). Sedation keeps you relaxed but awake.
3. **Imaging and Needle Insertion**: Using CT scans to plan the path, a small incision is made. A biopsy needle (fine for aspiration or larger core/trephine for tissue) is guided to the target—bone or disc—avoiding nerves and vessels. Approaches vary: transpedicular for lumbar, anterolateral for cervical, or posterolateral. You may feel pressure but should stay still.
4. **Sample Collection**: Tissue or fluid is extracted; multiple passes ensure adequacy. For discitis, samples go for culture and pathology.
5. **Closure**: The needle is removed, pressure stops any bleeding, and a bandage is applied—no stitches usually needed.
Ultrasound is faster and radiation-free but limited to accessible areas like cervical spine. CT is preferred for deeper lesions due to better accuracy.
## Risks and Complications
While safe, with complication rates under 1-10%, risks include:
- Bleeding, bruising, or hematoma (rarely needing transfusion).
- Infection at the site or in the bone/disc.
- Nerve damage or pain, especially near the spine.
- Pneumothorax (lung collapse) in thoracic biopsies.
- Tumor seeding along the needle track (rare, mainly with sarcomas).
- False negatives: Yield is about 48% for discitis biopsies, lower with prior antibiotics; may require repeat or open biopsy.
Accuracy ranges 68-97%, higher for malignancies than infections. Discuss risks with your doctor.
## Benefits of Imaging-Guided Spine Biopsy
This approach offers significant advantages:
- **Minimally Invasive**: Avoids general anesthesia and large incisions, reducing recovery time and costs compared to open biopsy.
- **High Precision**: Imaging ensures safe, accurate sampling, even in hard-to-reach areas.
- **Diagnostic Value**: Provides tissue for pathology, microbiology, and tailored treatment—essential for infections or cancers.
- **Outpatient-Friendly**: Often same-day discharge, with quicker results (1-2 weeks).
- **Lower Morbidity**: Compared to surgery, it has fewer wound issues and allows earlier therapy start.
For discitis, it identifies organisms in ~48% of cases, far better than non-invasive tests alone.
## Aftercare and Recovery
Post-procedure, you'll rest for a few hours with vital monitoring. Painkillers manage discomfort. Avoid driving or heavy activity for 24 hours; have someone stay with you overnight if sedated. Watch for signs of infection (fever, swelling) or bleeding, and contact your doctor if needed. Results are discussed in follow-up appointments. Full recovery is quick—most resume normal activities within days.
## Final Thoughts
Imaging-guided spine biopsies for discs or bones are game-changers in diagnosing spinal issues, balancing safety with effectiveness. While not without risks, their benefits often outweigh alternatives like open surgery. If you're facing persistent spine problems, talk to your specialist about whether this procedure fits your needs. Early diagnosis can lead to better outcomes—stay proactive about your health!