Unlocking Relief: Peripheral Nerve Stimulation as a Game-Changer for Chronic Pain
Living with chronic pain can feel like an endless battle. Millions of people worldwide grapple with conditions that disrupt daily life, from neuropathic pain after surgery to debilitating headaches or phantom limb sensations. Traditional treatments like medications, physical therapy, or even opioids often fall short, leading to frustration and dependency. But what if there was a way to target pain at its source—directly through the nerves? Enter peripheral nerve stimulation (PNS), a innovative neuromodulation therapy that's gaining traction as an effective, minimally invasive option for managing various pain conditions.
In this blog post, we'll dive into what PNS is, how it works, the pain conditions it treats, the procedure itself, its benefits and risks, and a glimpse into its future. Drawing from recent medical reviews and studies, we'll explore why PNS is becoming a beacon of hope for those who've tried everything else.
What is Peripheral Nerve Stimulation?
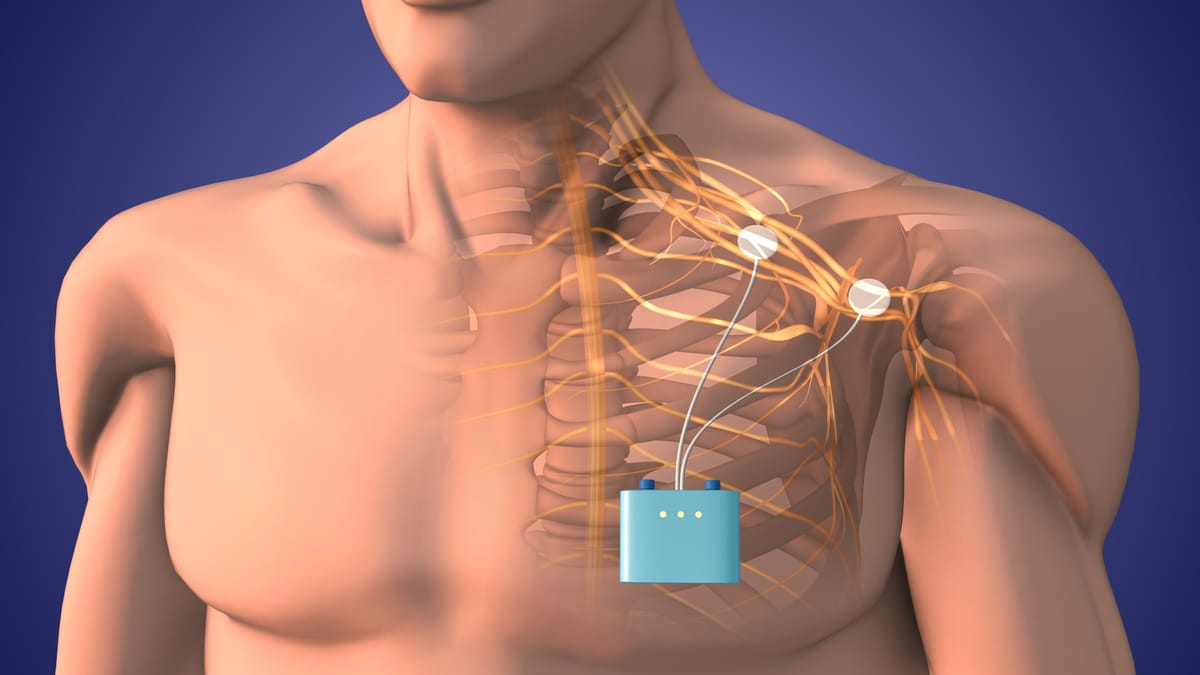
Peripheral nerve stimulation involves placing small electrodes near specific peripheral nerves—the nerves outside your brain and spinal cord—to deliver mild electrical pulses. These pulses aim to interrupt or modulate the pain signals traveling to your brain, essentially "hacking" the nervous system to reduce discomfort. Unlike spinal cord stimulation (SCS), which targets the central nervous system, PNS focuses on the peripheral nerves, making it more localized and often less invasive.
PNS has evolved significantly since its early days in the 1960s, with modern advancements including percutaneous (through-the-skin) leads and ultrasound-guided placements that minimize surgical risks. Today's systems often use external power sources, avoiding the need for implanted batteries and reducing complications like scarring or nerve damage seen in older cuff-style electrodes.
How Does PNS Work?
At its core, PNS operates on the gate control theory of pain, proposed by Melzack and Wall in 1965. This theory suggests that stimulating larger, non-pain-carrying nerve fibers (Aβ fibers) can "close the gate" on smaller pain-transmitting fibers (Aδ and C fibers), blocking pain signals from reaching the brain. Beyond that, PNS has anti-inflammatory effects: it reduces pro-inflammatory cytokines like IL-1β, IL-6, and TNF-α, calms overactive glial cells, and promotes healing by shifting immune responses.
Central brain pathways also play a role, with PNS influencing serotonin, dopamine, GABA, and glycine systems to enhance natural pain inhibition. In essence, it's not just masking pain—it's reprogramming how your body processes it.
Conditions Treated by PNS
PNS isn't a one-size-fits-all solution, but it's versatile, showing promise across a spectrum of pain conditions, particularly those involving neuropathic pain (pain from nerve damage).
Here's a breakdown of key applications based on recent evidence:
Neuropathic Pain (e.g., Post-Traumatic or Postsurgical Neuropathy): This is one of the strongest indications for PNS, with studies showing level II evidence (moderate quality) that about two-thirds of patients achieve at least 50% sustained pain relief. Conditions like nerve entrapment, post-stroke pain, and complex regional pain syndrome (CRPS) respond well, often better than traditional therapies.
Headaches and Migraines: For cluster headaches, trigeminal neuralgia, and occipital neuralgia, PNS targets nerves like the sphenopalatine ganglion or trigeminal branches. Reviews report 58-67% pain relief and reduced medication use, with a 61.3% response rate in meta-analyses.
Postamputation Pain (Phantom Limb or Residual Limb Pain): PNS provides 56-81% pain reduction, helping patients regain function and cut down on opioids. Some even report restored sensory feedback in the missing limb.
Chronic Pelvic Pain and Painful Diabetic Neuropathy: Tibial nerve stimulation offers level III evidence (fair quality) for pelvic pain, with over 50% relief at six months. For diabetic neuropathy, related techniques like percutaneous electrical nerve stimulation reduce pain scores significantly, though more PNS-specific studies are needed.
Postoperative and Other Pain: PNS shines in acute settings, like after knee surgery, reducing pain by 27-93% and sparing opioids. It's also explored for fibromyalgia, postherpetic neuralgia, and low back pain.
Overall, systematic reviews indicate PNS is effective for refractory cases, with sustained benefits in functional improvement and quality of life.
The PNS Procedure: What to Expect
Getting PNS typically starts with a trial phase. Under local anesthesia and ultrasound guidance, a doctor inserts thin leads near the target nerve—often percutaneously, without major surgery. These connect to an external stimulator for a test period (days to weeks) to assess effectiveness.
If successful, a permanent system is implanted, which might involve a small generator under the skin or remain external. The whole process is outpatient-friendly, with recovery in days. Advances like spiral electrodes improve stability and reduce migration risks.
Benefits and Risks
Benefits: PNS often leads to dramatic pain reduction, less reliance on drugs, better sleep, and enhanced daily function. It's reversible, customizable (adjust stimulation via a remote), and avoids the risks of central nervous system interventions like SCS. Many patients report long-term relief, with some studies showing benefits lasting a year or more.
Risks: While generally safe, potential issues include lead migration (common but fixable), infection (low, around 0-5%), skin irritation, or the need for revisions. Older systems had higher complication rates, but modern percutaneous tech has minimized these. Serious events like nerve damage are rare.
The Future of PNS
The field is buzzing with potential. High-frequency, paresthesia-free stimulation (no tingling sensation) and hybrid therapies (combining PNS with radiofrequency or botulinum toxin) are on the horizon. Researchers call for more high-quality randomized trials to refine indications, especially for diabetic neuropathy and postoperative pain. As hardware improves—think smaller, smarter electrodes—PNS could become a first-line option for many.
Final Thoughts
Peripheral nerve stimulation represents a shift toward targeted, tech-driven pain management that's empowering patients to reclaim their lives. If you're dealing with chronic pain and standard treatments aren't cutting it, talk to a pain specialist about PNS—it might just be the key to unlocking your relief.
Remember, while promising, it's not for everyone; personalized assessment is crucial.